X
An Integrated Network
Research
Training
Policy
Advocacy
Services & supports
Caregivers
People with ASD
Critical elements
Other elements
Major influences
Minor influences
A Model Research Roadmap
A diagram illustrates how each stage of screening research helps maintain progress towards improved diagnosis.
An Integrated Network
Relationships between services, training, policy, and advocacy reveals a unique role for research
Stages of Research
Each stage of research has a difference influence on the integrated network and on better outcomes
The CHAT+ Pilot Study
Applying the roadmap to 25 years of research invoving all versions of the CHecklist for Autism in Toddlers
Milestones
What distinguishes implementation and clinical research? Different participants, measures, and designs.
Resources Required
Each stage of research requires different training, funding models, partnerships, and scholarship.
Other Components
A structure that breaks progress down into manageable steps can help close persistent gaps identified via research.
Coming very soon
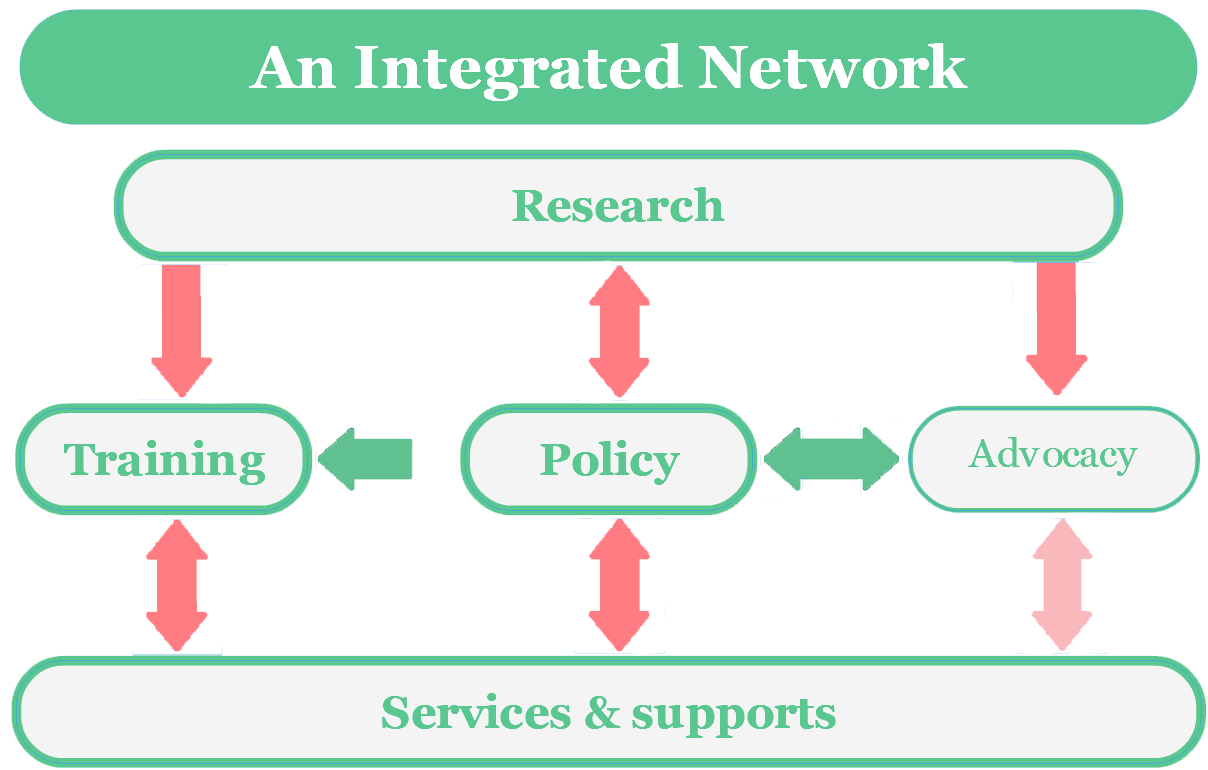 An integrated network
An integrated network
De-constructing the network of services, training, policy, and advocacy gives us a renewed appreciation of the unique role research can play in improving outcomes
January 28, 2019
Many different researchers, practitioners, and leaders aspire to achieve big outcomes. In the case of ASD identification, for example, we strive to accurately diagnose ASD as quickly as possible, regardless of a child's background. In fact, the Inter-Agency Autism Coordinating Committee (IACC) - the principle body for designing ASD research strategy in the US - has consistently included early detection as the first goal of each of its recent strategic plans, beginning more than 10 years ago. And many other goals within the IACC's strategic plan center on the goal of early detection, either as an important goal of research on causes and risk factors, or as an assumption of research promoting the benefits of early intervention.
It goes without saying that no single program will achieve a big outcome like the rapid and accurate diagnosis of ASD in all children affected. A broad roadmap that considers how research, services, training, and other elements influence one another within an integrated network can begin, however, to break these kinds of big outcomes down into smaller steps.
What might this integrated network look like? Let's take a look!
An integrated network
![]() Hover over to viewIt is simply unrealistic to expect that any single program of intervention or research could ever help us to reach such a big outcome, like timely and accurate diagnosis for all children with ASD. My previous work has outlined how research is simply one element of a roadmap to better outcomes. Research must be part of an integrated network that includes training, policy, and, increasingly, advocacy. All of these elements only influence outcomes through their impact on services and supports delivered to people with ASD, or their caregivers. Ideally, these services take the form of evidence-based practices (EBPs), delivered by individual, trained professionals, often working together as part of a program.
Hover over to viewIt is simply unrealistic to expect that any single program of intervention or research could ever help us to reach such a big outcome, like timely and accurate diagnosis for all children with ASD. My previous work has outlined how research is simply one element of a roadmap to better outcomes. Research must be part of an integrated network that includes training, policy, and, increasingly, advocacy. All of these elements only influence outcomes through their impact on services and supports delivered to people with ASD, or their caregivers. Ideally, these services take the form of evidence-based practices (EBPs), delivered by individual, trained professionals, often working together as part of a program.
Consider the evolution of EBPs. Just 10 years ago, there was no reasonable standard for the amount and quality of outcome research needed before a practice could be identified as evidence based. In other words, there was no clear roadmap to guide clinicians and program leaders who wanted to use outcome research to identify which new practices they should begin to use. Although there was consensus that clinicians should feel confident acting on the results of randomized, double-blind placebo control outcome research, it was not realistic to rely solely on this standard for evaluating the kinds of behavioral and educational interventions commonly used in community settings. Without such a roadmap, there was no clear path for intervention research to translate into outcomes through changes in in services. It was this gap in outcome research that first led to my work on EBPs, and my shift from leading programs of services to programs of training and research. This included helping to set a new standard for EBP that allows other kinds of research to be considered when designating a practice as evidence-based.
Many times, EBP cannot be translated into changes in services without taking other elements of the network into account, like training and policy. And this complex network break down easily and frequently. My detailed case study of a young man in behavioral crisis illustrates the many ways this can happen, with life-changing consequences for people living with ASD, and at tremendous cost to society. Some of these breakdowns are entirely avoidable given the evidence-based practices already available. For more than 20 years, I have sought to try to identify how to prevent such breakdowns, by translating research on diagnosis and treatment into specific programs in schools, hospitals, and universities. And for most of that time, I was directly accountable for the breakdowns that did occur, because I was directly delivering education and treatment, or because I was leading programs that delivered such services.
Multiple sectorsHome CommunityPhysical/Mental/Behavioral HealthPublic/Higher educationMultiple levelsLocal RegionalState NationalWe need clear roadmaps to navigate these complex inter-relationships. These relationships often span not just multiple elements (services, training, research, and policy), but often multiple sectors (health, education, and community services), and multiple levels (local, regional, state, and national). Several years ago, I tried to bring these complex relationships together in the design of a statewide autism training network. This network was carefully positioned to generate recommendations across agencies responsible for services, training, and policy, to gather data about progress directly from stakeholders, to pilot new programs of training, and to report directly to the state legislature.
Consider how a successful program of ASD screening must cut across disciplines, sectors, and agencies within a multi-level network. Screening can occur in community-based settings (like schools or pediatric clinics), but may require a specialist clinic at a regional hospital to complete the diagnostic assessment, or a policy decision at the state level that ensures that screenings will be properly reimbursed. Perhaps each of these decisions is spurred by a recommendation at the national level to conduct universal ASD screening, delivered by a panel of experts from a professional practice organization like the American Academy of Pediatrics.
I first tried to navigate such a network with respect to ASD screening more than 20 years ago, when I developed and delivered a program to try to train pediatricians across Montreal to use the CHAT. Later, I designed a web-based roadmap that was specifically intended to help parents and professionals navigate the system of services by drawing on the expertise of a statewide Act Early team, with the ultimate goal of gathering data on service gaps that would shape a statewide plan. These and other lessons learned were integrated into my 2013 review. This review concluded with a recommendation that we begin by constructing roadmaps that focus on a subset of specific, pivotal outcomes, like improved identification of ASD through early screening and diagnosis.
Understanding the complementary roles of individual professionals and agencies within the network
Every element within this roadmap seeks different outcomes and adopts different definitions of progress. In the case of ASD screening, a researcher pursuing a specific line of inquiry might define progress in term of increased understanding of the early indicators of ASD. A professional implementing a specific practice with a particular student, patient, or client might define progress in terms of access to a new screening tool. A leader promoting the adoption of a large-scale screening program might define progress in terms of improved access for an entire population of people with ASD. We hope that these differences will ultimately converge in the big, overarching goal for our science that our society adopts, although our recent review revealed no examples of specific research studies designed to achieve or to document a state or national impact (Doehring, 2019).
Such a roadmap can help to define these very specific, often complementary, and inter-related roles of individuals within different agencies and sectors, at different levels of the network. Consider the example of ASD screening undertaken by a community-based pediatrician. A pediatrician who reads an article about a promising new screening tool usually cannot just begin to successfully implement the practice through the services they deliver themselves. They must often collaborate with others in a program of services (e.g., they consider the results of the ASD screening with the results of other screening tools completed by nurse practitioner before making a specific referral). Sometimes the practice requires coordination with professionals in another program (e.g., screening might only be considered appropriate if another program is able to provide more specialized diagnostic evaluations as needed). Sometimes the practice is enhanced by statewide training offered through a university-based program. Several programs I have helped to develop and implement focused on early identification sought to capitalize on the complementary roles of different professionals (like an initiative to train nurse practitioners to effectively diagnose ASD in less complex cases) and agencies (like an initiative to train community-based clinics outside of urban regions to reliably diagnose ASD in less complex cases).
One of the biggest challenges is the fact that many professionals have limited, meaningful experience in other sectors, or focused on multiple elements. For example, many professionals spend most or all of their professional career in one kind of agency (in a hospital or a school or a university or in government) focused on one element (services or training or research or policy). This becomes more challenging as research seeks to evolve beyond the laboratory to address training and services, or to reach beyond the university to include school and community resources, or beyond the local level to reach state or federal policymakers. Even when adopting specific strategies like collective impact that take advantage of the strengths of each partner, professionals trying to work across elements or sectors are much less likely to understand the opportunities or challenges faced by their collaborators.
And many professionals have limited experience in leading programs, especially through significant periods of growth and change. Even under the best of conditions, developing and implementing large scale change is a challenge without strong and experienced leadership. Problem leaders will struggle to achieve simple expansion or improvements in services, let alone true innovation.
As a result, trying to promote an emerging practice across different sectors, elements, or levels is like running a relay race of undetermined length and difficulty, with unidentified runners who are partially blindfolded and trying to hand off a greased baton (Doehring, 2013). Perhaps that is why we have no examples of a program of research designed intentionally and implemented successfully to demonstrate change on a regional level (Doehring, 2019). But with a roadmap that clearly defines the elements of the network and how they interact, we can at least to imagine such program, and perhaps begin to recruit our runners and train for our race.
Related Content
On this site
A Model Research Roadmap
A diagram illustrates how each stage of screening research helps maintain progress towards improved diagnosis.
An Integrated Network
Relationships between services, training, policy, and advocacy reveals a unique role for research
Stages of Research
Each stage of research has a difference influence on the integrated network and on better outcomes
The CHAT+ Pilot Study
Applying the roadmap to 25 years of research invoving all versions of the CHecklist for Autism in Toddlers
Milestones
What distinguishes implementation and clinical research? Different participants, measures, and designs.
Resources Required
Each stage of research requires different training, funding models, partnerships, and scholarship.
Other Components
A structure that breaks progress down into manageable steps can help close persistent gaps identified via research.
Coming very soon
X
My Related Publications
 ( 2019). The Impact of ASD Research on National Policy (Ch. 9). In Volkmar, F. (Ed.). Autism and Pervasive Developmental Disorders (3rd Ed.). Cambridge University Press, Cambridge, UK.
( 2019). The Impact of ASD Research on National Policy (Ch. 9). In Volkmar, F. (Ed.). Autism and Pervasive Developmental Disorders (3rd Ed.). Cambridge University Press, Cambridge, UK.
 (2011). With Brian Reichow, Dominic Cicchetti, & Fred Volkmar F. (Eds.). Evidence-Based Practices and Treatments for Children with Autism. Springer-Verlaug, New York, NY.
(2011). With Brian Reichow, Dominic Cicchetti, & Fred Volkmar F. (Eds.). Evidence-Based Practices and Treatments for Children with Autism. Springer-Verlaug, New York, NY.
![]() (2010). With Megan Ott and Susan Levy. Early Autism Screening and Identification Clinic (EASI): A Nurse Practitioner & Physician Clinic Model. National Autism Conference. State College PA.
(2010). With Megan Ott and Susan Levy. Early Autism Screening and Identification Clinic (EASI): A Nurse Practitioner & Physician Clinic Model. National Autism Conference. State College PA.

